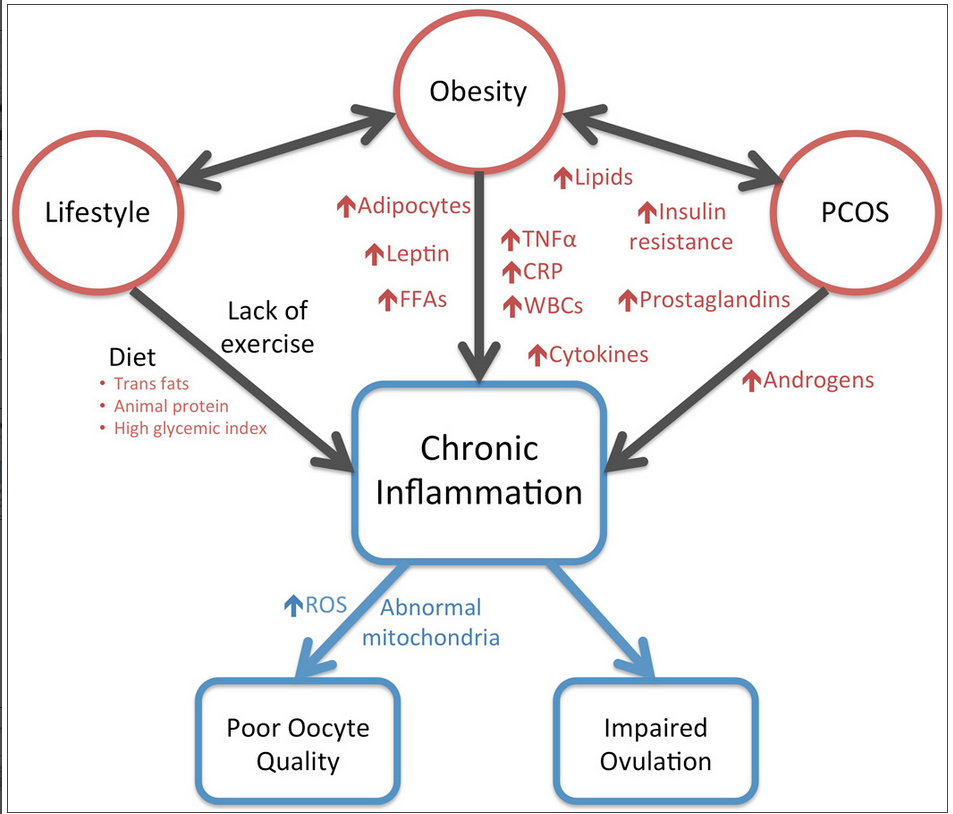
Inflammation, PCOS, and Your Weight
Contrary to what you may think, body fat in PCOS women is not simply an inert storehouse of unused calories encasing your body and organs.
Actually, your fat cells are metabolically very active and are intimately involved with your symptoms and problems. For example, they produce hormones (such as estrogen) and other signaling molecules that have far-reaching effects throughout your body.
Free PCOS Newsletter
The signals that are sent and received by your fat cells will influence how much fat you retain and how easy or difficult it will be for you to lose weight. Some of these signals are created as the result of inflammation.
A number of studies indicate that PCOS women who are overweight tend to be in a state of chronic inflammation.
Even adolescents with PCOS symptoms of high insulin and testosterone have elevated white blood counts, suggesting that the immune system is aroused and an inflammatory process may be occurring. The white blood count is elevated even more when birth control pills are taken.
Chronic inflammation appears to play an under-recognized but central role in the pathology of PCOS and obesity.
Read these Important Articles
C-Reactive Protein (CRP) Commonly Elevated in PCOS
 PCOS Women Have More Inflammation
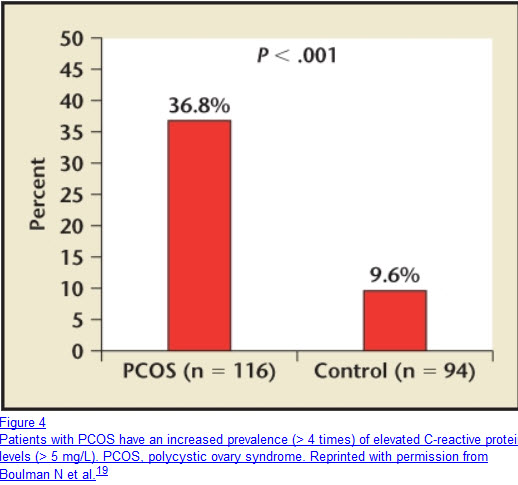
PCOS Women Have More InflammationC-reactive protein (CRP) is a protein that is a general indicator of inflammation and is associated with being overweight. CRP is a fairly common blood test that you can get from your doctor. A high level of CRP is a strong predictor of future cardiovascular disease and stroke.
In a study at the Rambam Medical Center in Israel, 36.8% of PCOS women had elevated CRP whereas only 9.6% non-PCOS women had elevated levels. Estrogen, which may be in excess in some PCOS women, is one of numerous factors that can increase CRP.
Study Links Diet to Inflammation and Diabetes
Researchers involved in the Nurses Health Study have discovered a dietary pattern that is very closely related to the degree of inflammation and the incidence of diabetes.
As you know, PCOS has an inflammatory component that worsens your symptoms and substantially increases the risk of developing diabetes.
The study revealed that women whose diet was high in sugar-sweetened soft drinks, refined grains, diet soft drinks, and processed meat had much higher levels of inflammation and incidence of diabetes. In fact, the women with the highest consumption of these foods were 2.5 times as likely to develop diabetes compared to women who had the lowest consumption of these items. The women with the most inflammation and diabetes also ate fewer vegetables.
If you're still consuming soft drinks, refined grains and processed meat, it's time for you to stop and think. It's well-known that if you have PCOS, you already have a much higher risk of getting diabetes than other women. By eating these foods, you're only making matters worse. We urge you to improve your diet immediately.
This study explains why we do not include these foods in The Natural Diet Solution to PCOS and Infertility e-book…and why we stress the importance of eating more vegetables.
What Is Inflammation?
Inflammation is part of your body's response to injury or infection. It is a byproduct of the body's attempt to heal itself. Usually, you are aware of inflammation by its classic signs of redness, heat, swelling and pain. However, there is a very complex, hidden, powerful biochemical process that results in these classic signs of inflammation.
Inflammation is not always as obvious as pain or swelling. It can occur at a low, unnoticeable level. This is referred to as sub-clinical, chronic inflammation. In other words, the inflammatory biochemical process is occurring, but you are not aware of it. Chronic, low-grade inflammation is what we are concerned about in dealing with PCOS and weight problems.
Body Fat Causes Inflammation
You can think of your fat cells as an endocrine and secretory organ, just like your ovaries, thyroid, adrenal glands, liver, hypothalamus, or any other organ or gland in your body. Fat cells produce a bewildering array of biochemicals that influence what goes on in your body.
One family of biochemicals produced by your fat cells are "cytokines", many of which are involved in the inflammatory process. They include leptin, adiponectin, tumor necrosis factor alpha (TNF-alpha), interleukin-6 (IL-6), to name a few. Most cytokines promote inflammation while some others inhibit inflammation.
The more fat cells you have, especially around your middle, the more cytokines you will produce and the more likely it is that you are promoting inflammation.
Fat-Immune System-Inflammation Link
Your fat cells increase inflammation in another way, by attracting a type of white blood cell known as a macrophage, which produces inflammatory cytokines. Macrophages are scavenger cells. Their job is literally to gobble up foreign organisms and cellular debris.
Macrophages seem to be drawn to body fat because fat cells tend to leak and break open, especially in people with abdominal obesity. Macrophages move into the leaky fat tissue in order to clean up debris and then they themselves begin to release inflammatory factors. Macrophages appear to be a major contributor to inflammation.
SOCS and Leptin Resistance
To limit the damage produced by inflammation, your body produces anti-inflammatory biochemicals that are triggered by the inflammation itself. This is a compensating mechanism that attempts to maintain a balance in the healing process.
When pro-inflammatory cytokines enter a cell to initiate or promote a biochemical processes to increase the inflammatory response, the cell simultaneously produces anti-inflammatory chemicals called "suppressors of cytokine signaling", or simply "SOCS". SOCS molecules suppress the cell's response to inflammatory cytokines. Two SOCS molecules, SOCS-1 and SOCS-3, are able to interfere with a cell's ability to respond to leptin, which increases leptin resistance. SOCS-3 also blocks the response to insulin, which increases insulin resistance.
Some researchers believe that SOCS production is an important cause of leptin resistance and consequently contributes to the development of obesity.
Some with PCOS May Have a Problem with Resistin
Fat cells and macrophages (a type of white blood cell) produce a hormone called resistin. Resistin appears to cause tissues -- especially the liver -- to be less sensitive to the action of insulin and thus lead to increased blood sugar levels. There is a strong association between elevated levels of resistin and obesity and diabetes.
Resistin is a potent stimulator of inflammation. In experiments, increased levels of resistin also appear to induce increased SOCS-3.(18) As we said, SOCS-3 contributes to leptin resistance and insulin resistance.
The amount of body fat you have may also increase resistin. While resistin in produced by fat cells, it is also produced by the macrophages that are attracted to debris leaking from fat cells. Increased macrophage activity could lead to more resistin.
Although resistin levels are not elevated in all PCOS women, these women appear to be more inclined to produce resistin than those without PCOS.
Sources:
Schulze, MB et al, Dietary pattern, inflammation, and incidence of type 2 diabetes in women, Am J Clin Nutr. 2005 Sep;82(3):675-84
Kelly, CC et al, Low grade chronic inflammation in women with polycystic ovarian syndrome, J Clin Endocrinol Metab. 2001 Jun;86(6):2453-5
Mohlig, M et al, The polycystic ovary syndrome per se is not associated with increased chronic inflammation, Eur J Endocrinol. 2004 Apr;150(4):525-32
Puder, JJ et al, Central fat excess in polycystic ovary syndrome: relation to low-grade inflammation and insulin resistance, J Clin Endocrinol Metab. 2005 Nov;90(11):6014-21
Orio Jr., F et al, The increase of leukocytes as a new putative marker of low-grade chronic inflammation and early cardiovascular risk in polycystic ovary syndrome, J Clin Endocrinol Metab. 2005 Jan;90(1):2-5
Ibanez, L et al, High neutrophil count in girls and women with hyperinsulinaemic hyperandrogenism: normalization with metformin and flutamide overcomes the aggravation by oral contraception, Hum Reprod. 2005 Jun 23; [Epub ahead of print]
Sonnenberg, GE et al, A novel pathway to the manifestations of metabolic syndrome, Obes Res. 2004 Feb;12(2):180-6
Miner JL, The adipocyte as an endocrine cell. J Anim Sci. 2004 Mar;82(3):935-41
Trayhurn, P et al, Signalling role of adipose tissue: adipokines and inflammation in obesity, Biochem Soc Trans. 2005 Oct;33(Pt 5):1078-81
Skurk, T et al, Production and release of macrophage migration inhibitory factor from human adipocytes, Endocrinology. 2005 Mar;146(3):1006-11
Weisberg, SP et al, Obesity is associated with macrophage accumulation in adipose tissue, J Clin Invest. 2003 Dec;112(12):1796-808
Bjorbaek, C et al, Identification of SOCS-3 as a potential mediator of central leptin resistance, Mol Cell. 1998 Mar;1(4):619-25
Bjorbaek, C et al, The role of SOCS-3 in leptin signaling and leptin resistance. J Biol Chem. 1999 Oct 15;274(42):30059-65
Farrell, GC, Signalling links in the liver: Knitting SOCS with fat and inflammation, J Hepatol. 2005 Jul;43(1):193-6
Emanuelli, B et al, SOCS-3 inhibits insulin signaling and is up-regulated in response to tumor necrosis factor-alpha in the adipose tissue of obese mice, J Biol Chem. 2001 Dec 21;276(51):47944-9
Senn, JJ et al, Suppressor of cytokine signaling-3 (SOCS-3), a potential mediator of interleukin-6-dependent insulin resistance in hepatocytes, J Biol Chem, 2003 Apr 18;278(16):13740-6
Silswal, N et al, Human resistin stimulates the pro-inflammatory cytokines TNF-alpha and IL-12 in macrophages by NF-kappaB-dependent pathway, Biochem Biophys Res Commun. 2005 Sep 9;334(4):1092-101
Bokarewa, M et al, Resistin, an adipokine with potent proinflammatory properties, J Immunol. 2005 May 1;174(9):5789-95
Steppan, CM et al, Activation of SOCS-3 by resistin, Mol Cell Biol. 2005 Feb;25(4):1569-75
Lehrke, M et al, An inflammatory cascade leading to hyperresistinemia in humans, PLoS Med. 2004 Nov;1(2):e45. Epub 2004 Nov 30
Seow, KM et al, Serum and adipocyte resistin in polycystic ovary syndrome with insulin resistance, Hum Reprod. 2004 Jan;19(1):48-53
Boulman, N et al, Increased C-reactive protein levels in the polycystic ovary syndrome: a marker of cardiovascular disease, J Clin Endocrinol Metab. 2004 May;89(5):2160-5
De Maat, MP et al, Determinants of C-reactive protein concentration in blood, Ital Heart J. 2001 Mar;2(3):189-95
Get Answers to your Questions about
- Fertility
- Weight Control
- Hair Loss
- Stress
- Unwanted Hair
- Acne...and more!
FREE PCOS Report
and Newsletter

Your email is safe with us. We respect your privacy, and you may unsubscribe at any time.
Recent Articles
-
PCOS Long Journey to The Happy End
Apr 30, 18 07:24 PM
Hi Girls, Maybe my story will have one day a good end but I am not there yet. Until I was 31 years old I lived my dream, having lovely husband, good -
PCOS and Miscarriage
Apr 17, 18 04:03 PM
Proper diet and natural supplements can help the body maintain a pregnancy through successful delivery.
-
How to Deal with PCOS and Stress
Apr 04, 18 04:19 PM
Your body has a natural capacity to heal itself if you provide it with the necessary tools.