Does Your Thyroid Hold the Key to PCOS and Polycystic Ovaries?
Do you have PCOS -- and feel fatigued, depressed, or anxious? Are you losing hair or having trouble losing weight? And, have the doctors found nothing wrong with you?
If so, you may have a problem with your thyroid gland and hormones.
Free PCOS Newsletter
About 10% of women have or will develop thyroid disease, especially hypothyroidism. Up to 60% of women are unaware they have the disease. Women with polycystic ovary syndrome are no exception.
There is some evidence that infertile PCOS women have a higher prevalence of thyroid dysfunction than other women.
So this is a potential problem that is lurking under the surface and could be a factor in why you're not ovulating, can't become pregnant, can't lose weight, feel sluggish and depressed, and have hair problems.
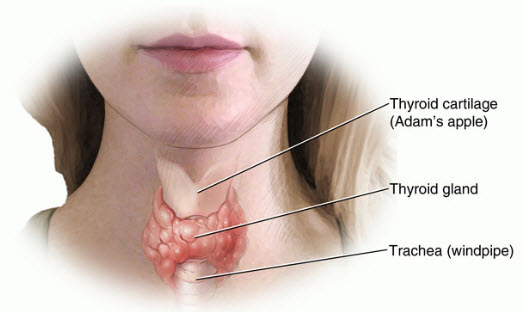
The thyroid gland is located at the base of your neck in front of your windpipe. It makes, stores, and releases two very important hormones - T4 (thyroxine) and T3 (triiodothyronine). Thyroid hormones control your metabolic rate, the rate at which every part of your body works. If there is not enough thyroid hormone in your bloodstream, your metabolism slows down. This is called hypothyroidism.
How Thyroid Hormones Work
- The pituitary gland (underneath the brain) releases a hormone called TSH (thyroid stimulating hormone, which tells the thyroid to produce hormones.
- The thyroid then makes T4, the major thyroid hormone, which in not active.
- The body converts T4 into T3, which is the active hormone that stimulates the cells to work.
- Some T4 is also converted into rT3 (reverse T3), which is not an active hormone. Too much rT3 blocks the action of regular T3.
Hypothyroidism and PCOS
The circulating thyroid hormones have a profound effect on your tissues and organs. For example, they govern your metabolic rate. So if your thyroid is sluggish, you might have trouble losing weight.
It's also known to deeply affect your reproductive system. You also need optimal thyroid hormone function to ovulate and have a baby.
Abnormally low levels of thyroid hormones ("hypothyroidism") are associated with ovarian cysts and an increase in ovarian size. Some research suggests that thyroid hormone replacement reduces these problems.
Hypothyroidism is also associated with changes in many other signaling molecules, including:
- Sex hormone binding globulin (SHBG)
- Prolactin
- Estradiol (an estrogen)
- Progesterone
- Testosterone
- Luteinizing hormone (LH)
- Follicle stimulating hormone (FSH).
All of these hormones and molecules may be out of balance if you have PCOS. (Could your thyroid be involved?)
Thyroid Hormones Are Required for Ovulation and Pregnancy
A major effect of abnormal thyroid levels is changes in ovulation and menstruation. Ovulation may be impaired by changes in the production of: sex hormone binding globulin (SHBG), follicle stimulating hormone (FSH), estrogen, and androgens.
The body compensates by altering the production of thyroid releasing hormone (TRH). The changes in TRH will affect the feedback loop between the hypothalamus, pituitary, and the ovary, leading to changes in ovulation and menstruation.
Early stages of thyroid dysfunction (before symptoms are obvious) can lead to subtle changes in ovulation and endometrial receptivity, which then may have profound effects on fertility.
Too Much Estrogen -- Does It Lead to Hypothyroidism?
A few physicians will prescribe some thyroid hormone when they prescribe an estrogen medication.
Why would they do that?
Extra estrogen causes an increase in the amount of circulating thyroid binding globulin (TBG). TBG is a protein the "soaks up" freely circulating thyroid hormone, turning it from "free" thyroid hormone into "bound" thyroid hormone. So even though your thyroid levels might be "normal", less of what you have is active.
This shift away from "free" hormone to "bound" hormone contributes to hypothyroid symptoms such as weight gain, less energy and dry skin.
Many women with polycystic ovarian syndrome may have a predisposition to "estrogen dominance".
Excessively high levels of estrogen may diminish the effectiveness of your thyroid hormones. Therefore, a full assessment of your thyroid function and sex hormones is suggested if you are having trouble managing your PCOS symptoms.
The SHBG (Sex Hormone Binding Globulin) - Testosterone Link
An underactive thyroid gland can lead to a reduction of sex hormone binding globulin, which may increase in free testosterone. Free testosterone is one of the factors contributing to PCOS symptoms -- infertility, polycystic ovaries, hirsutism, male pattern hair loss, and acne.
You probably know about testosterone. A lot of people say too much testosterone is why you have PCOS and that's why you take birth control pills or "anti-androgen" medications.
But what regulates the testosterone floating around in your body? That's were SHBG comes in.
SHBG is like Velcro. It sticks to certain hormones such as testosterone. When this happens, the testosterone is rendered inactive. So you have some testosterone that is active, and some that is inactive. The inactive hormone has no hormonal effect on your body.
So SHBG is one of the mechanisms by which your body regulates testosterone.
But what if your SHBG is too low? In this case, you have more active testosterone hormone than you need and you end up with symptoms of PCOS like unwanted hair growth or acne.
Liver Disease - Hypothyroidism Link
So it's clear that you want to have a normal level of SHBG. SHBG is created mostly in your liver. But if your liver is not working very well, it may not produce enough SHBG. One problem is that possibly up to one-half of all PCOS women have a fatty liver disease called NAFLD. The worse your fatty liver disease is, the lower your SHBG is likely to be.
And interestingly, Seoul National University Hospital in South Korea has recently reported a close association between hypothyroidism and NAFLD. Could hypothyroidism contribute to NAFLD in some way, and thus cause SHBG to decrease? It's an intriguing question we might explore another time.
Let's Summarize Thyroid Impact on PCOS
First, if you have abnormal thyroid hormone function, it is much harder to solve your PCOS problems and improve your fertility.
Second, your body is an interconnected web of messaging systems, each one affecting the others. PCOS is clearly a malfunction of multiple messaging systems and organs and glands.
So you can't just take birth control pills and call it a day. PCOS is way, way more complicated than that. You will have to dig a little deeper. For example, if you have a thyroid disorder, birth control pills won't fix that.
Third, get a proper assessment of your thyroid function from your doctor. You may discover a problem you were not aware of.
Related Articles
Sources:
Source: Nutriton & Healing Newsletter, Jonathan Wright, MD, March 2004, p.4
Ghosh, S et al, Subclinical hypothyroidism: a determinant of polycystic ovary syndrome, Horm Res, 1993, 39(1-2):61-6
Wu X, et al, [Functional states of pituitary-ovary, adrenal and thyroid axes in women with polycystic ovarian syndrome], Zhonghua Fu Chan Ke Za Ahi, 1998, 33(3):153-6
Iptisam IM et al, Effect of thyroid hormone replacement therapy on ovarian volume and androgen hormones in patients with untreated primary hypothyroidism. Ann Saudi Med. 2011 Mar-Apr; 31(2): 145-151.
Chung GE, Non-alcoholic fatty liver disease across the spectrum of hypothyroidism. J Hepatol. 2012 Jul;57(1):150-6.
Shin JY et al, Serum sex hormone-binding globulin levels are independently associated with nonalcoholic fatty liver disease in people with type 2 diabetes. Diabetes Res Clin Pract. 2011 Oct;94(1):156-62.
Morgante G et al. Alterations in thyroid function among the different polycystic ovary syndrome phenotypes. Gynecol Endocrinol. 2013 Nov;29(11):967-9.
Get Answers to your Questions about
- Fertility
- Weight Control
- Hair Loss
- Stress
- Unwanted Hair
- Acne...and more!
FREE PCOS Report
and Newsletter

Your email is safe with us. We respect your privacy, and you may unsubscribe at any time.
Recent Articles
-
PCOS Long Journey to The Happy End
Apr 30, 18 07:24 PM
Hi Girls, Maybe my story will have one day a good end but I am not there yet. Until I was 31 years old I lived my dream, having lovely husband, good -
PCOS and Miscarriage
Apr 17, 18 04:03 PM
Proper diet and natural supplements can help the body maintain a pregnancy through successful delivery.
-
How to Deal with PCOS and Stress
Apr 04, 18 04:19 PM
Your body has a natural capacity to heal itself if you provide it with the necessary tools.





