If You Have PCOS, You May Also Have Non-Dipping Blood Pressure
Well, here's a piece of news about PCOS that isn't welcome. But awareness is better than ignorance, so here it is.
I'm sure you know that high blood pressure is unhealthy, and that it can contribute to cardiovascular problems later on.
Heart health is an important issue for everyone, but especially for you. Cedars-Sinai Medical Center in Los Angeles has reported that postmenopausal women with a history of polycystic ovary syndrome a 3.3-fold higher risk of cardiovascular death or a heart attack. So anything you can do to reduce this risk is a good idea.
Free PCOS Newsletter
Which brings us back to blood pressure. There's something interesting about blood pressure. It doesn't stay the same. For example, a mildly stressful visit to your doctor might elevate your blood pressure. Or, if you're a very overweight person, you might expect your blood pressure to be higher than in someone who is lean.
Also, you would expect it to drop if you're having a pleasant night's sleep.
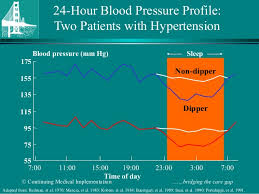
But Fatih University Medical School in Turkey has discovered something different about women with polycystic ovarian syndrome. Unlike other women, your blood pressure tends to drop less than 10% at night compared to the daytime. This is called a "non-dipping" blood pressure pattern.
In this study, 168 women with PCOS were compared to 50 other women. The prevalence of non-dipping blood pressure was 43.4% in PCOS patients but only 3.9% in the other group.
In other words, it appears you're ten times more likely to be a non-dipper than someone without polycystic ovarian syndrome. Moreover, even lean and younger PCOS women were found to be non-dippers.
Besides the increased risk of heart attack, non-dippers also experience more organ damage from the incessant blood pressure. In fact, a non-dipping pattern is a predictor of future cardiovascular problems.
The trouble with a non-dipping pattern is that your doctor is not in your bedroom conducting a blood pressure test while you're asleep. So there's no direct way to know if you're a non-dipper.
The cause of the non-dipping pattern is somewhat unclear. However, there is speculation it could have something to do with a form of inflammation called oxidative stress, or possibly insulin resistance. An increased waist circumference may also be an indicator of non-dipping risk.
If You Have PCOS and High Blood Pressure
OK, so where do we go from here?
Take a blood pressure medication for some number of years? A problem with medications is that they have side effects. Not an ideal solution.
You could avoid salt. But salt reduction does not get rid of high blood pressure for everyone.
Or you could try the DASH diet, which is approved for high blood pressure by the health authorities. This would be a step in the right direction but may not take you far enough.
One of your goals should be to reduce chronic inflammation, which is common in PCOS, and to reduce your waist circumference.
You can do this by greatly increasing your consumption of vegetables. Five servings per day is recommended. Cut your consumption of grains and reduce legumes; replace these with vegetables. Have some nuts and seeds. Go easy on the fruit. Stay completely away from processed foods and added sweeteners.
And start exercising on a regular basis (5 days a week at least).
I know you've heard these diet and exercise recommendations before. It bears repeating because you don't want to be a non-dipper!
Related Articles
Sources:
Kargili A, Association of polycystic ovary syndrome and a non-dipping blood pressure pattern in young women, Clinics (Sao Paulo). 2010 May;65(5):475-9.
Shaw LJ et al, Postmenopausal women with a history of irregular menses and elevated androgen measurements at high risk for worsening cardiovascular event-free survival: results from the National Institutes of Health--National Heart, Lung, and Blood Institute sponsored Women's Ischemia Syndrome Evaluation, J Clin Endocrinol Metab. 2008 Apr;93(4):1276-84.
Get Answers to your Questions about
- Fertility
- Weight Control
- Hair Loss
- Stress
- Unwanted Hair
- Acne...and more!
FREE PCOS Report
and Newsletter

Your email is safe with us. We respect your privacy, and you may unsubscribe at any time.
Recent Articles
-
PCOS Long Journey to The Happy End
Apr 30, 18 07:24 PM
Hi Girls, Maybe my story will have one day a good end but I am not there yet. Until I was 31 years old I lived my dream, having lovely husband, good -
PCOS and Miscarriage
Apr 17, 18 04:03 PM
Proper diet and natural supplements can help the body maintain a pregnancy through successful delivery.
-
How to Deal with PCOS and Stress
Apr 04, 18 04:19 PM
Your body has a natural capacity to heal itself if you provide it with the necessary tools.





